Translate this page into:
Depression, Anxiety, and Stress Levels among Medical Students and Interns in a Medical College of Kolkata: A Cross-Sectional Study
*Corresponding author: Ankush Banerjee, Department of Community Medicine, Medical College, Kolkata, West Bengal, India. ankush.banerjee20@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Chakraborty A, Jha A, Banerjee A, Banerjee N, Saha D, Das A. Depression, Anxiety, and Stress Levels among Medical Students and Interns in a Medical College of Kolkata: A Cross-Sectional Study. J Compr Health. doi: 10.25259/JCH_18_2024
Abstract
Background:
Medical students and interns are the future backbone of the medical fraternity and healthcare system in India. There have been increasing concerns raised on their mental health and wellbeing over the past decade.
Objectives:
This study thus assessed the presence of depression, anxiety and stress among undergraduate medical students and interns in a medical college of Kolkata and elicit its associates.
Material and Methods:
This cross-sectional study was conducted among 340 medical students and interns of Medical College, Kolkata from November 2023 to January 2024. The validated DASS-21 was utilized to assess depression, anxiety and stress among the study participants selected by stratified random sampling across all batches. Data were analyzed using SPSS.
Results:
Depression, anxiety and stress was present among 109 (32.0%), 138 (40.6%) and 46 (13.5%) participants. Chi-square revealed female gender to be associated with the presence of anxiety and stress. Substance usage was detected as an important predictor for the presence of stress among the study participants.
Conclusion:
Utmost care should be taken for the betterment of mental health and well-being of medical students. Awareness generation and one-to-one counseling sessions through motivation should be conducted especially for the vulnerable participants. Parents and peers can act as buffers to help those students to cope with stressful circumstances.
Keywords
Anxiety
Depression
Medical students
Interns
Stress
INTRODUCTION WITH OBJECTIVES
The Indian Medical Graduate Degree, Bachelor of Medicine, and Bachelor of Surgery (MBBS) has one of the toughest and most competitive curricula across the globe, especially due to its vastness and working intensity. MBBS education in India often involves academic classes and clinical rotations across various non-clinical, para-clinical, and clinical subjects.1,2 Medical education has high demand across India and often has a high impact on the mental health and well-being of students of its students, which leads to increased levels of psychological distress and makes them vulnerable to high levels of negative affective states. Long working and study hours, environments not ideally suited to learning, sleep deprivation, as well as factors disturbing everyday personal life are common during this period.3
A review of the literature has revealed an increasing incidence of psychological distress among medical students in recent times. There has been an increase in suicide rates among medical students in India, as evidenced by the occurrence of 358 suicides in the past decade among medical students in India.4 Raja et al. conducted a study in a medical college in southern India and reported that 59%, 43%, and 11% suffered from depression, anxiety, and stress, respectively.5
Digital learning has now become highly integrated into the medical education curriculum in India. Students often consult the internet and database platforms to learn the recent advances in the subject, which might not be present in textbooks. The pressure of competitive examination and its preparation often leads to spending long hours on tablets and smartphones. This, in turn, leads to sleep deprivation, which hampers the mental health and well-being of students. Deranged mental health has the potential to reduce the academic performance of an individual, which can initiate a vicious cycle of severe mental breakdown, leading to negative consequences.
Various standardized and validated mental health screening tools are available across the internet, but they mostly concentrate on single aspects of psychological distress. The depression, anxiety, and stress scale-21 (DASS-21) scale forms a composite measure that assesses three domains of psychological distress: Anxiety, depression, and stress.6
Although many studies have been conducted on Indian medical students regarding psychological distress, they have mainly focused on a single domain. Moreover, relevant aspects of stress models need further exploration considering the current scenario. Against this backdrop, this study aimed to assess the magnitude of depression, anxiety, and stress levels among medical students and interns in a medical college in West Bengal and elicit its associates, if any.
MATERIAL AND METHODS
This cross-sectional study was conducted among medical students and interns at Medical College and Hospital, Kolkata, from November 2023 to January 2024. Participants who did not provide written informed consent and were absent throughout the study period were excluded from the study.
Sampling
A systematic review among medical students in India by Sarkar et al.7 revealed the pooled prevalence of anxiety among Indian medical students to be 34.5%. Considering P = 0.345, Z1-a/2 = 1.96, relative error of precision to be 15%, the minimum sample size estimated using Cochran’s formula came to be 337.
Stratified random sampling was done to select the study participants. There were in total 5 batches of medical students comprising 1st year, 2nd year, 3rd year, and 4th year and internship phase. In each phase, there were 250 students. Thus, in total, there were 1250 students. Number of participants to be selected from each batch was done as per proportionate allocation. Thus, from each batch, 68 students were selected, which led to a total sample size of 340.
Data collection, study tools, and parameters used
The study was conducted through face-to-face interviews with the study participants with the help of a pre-designed structured questionnaire. The questionnaire was pre-tested among 30 medical students in a different study setting who were not included in the final study. The reliability of the questionnaire was estimated using Cronbach’s alpha coefficient (a = 0.74). Subject experts assessed the face and content validity of the questionnaire. The questionnaire consisted of the following domains:
Sociodemographic characteristics of the study participants such as age, gender, religion, residence, educational status of parents, type of family, socioeconomic status, and presence of family problems,
Behavioral characteristics such as substance usage and smartphone usage.
Presence of psychological distress among the study participants was assessed using the DASS-21 items.6,8 The DASS-21 screens the following three domains of psychological distress: anxiety, depression, and stress. There are three subscales for three respective domains, with each subscale consisting of seven items. Scores achieved on the DASS-21 needed to be multiplied by 2 to achieve the final score. Thus, the total scores in each domain ranged from 0 to 42. The cutoff scores and their respective categories for each domain are as follows:
Depression: Normal (scores: 0–9), mild (10–13), moderate (14–20), severe (21–27), and extremely severe (28+)
Anxiety: Normal (scores: 0–7), mild (8–9), moderate (10–14), severe (15–19), and extremely severe (20+)
Stress: Normal (scores: 0–14), mild (15–18), moderate (19–25), severe (26–33), and extremely severe (34+).
Data analysis
Data were analyzed using Microsoft Excel (v.2019) and Statistical Package for the Social Sciences v.20, IBM Corp. USA. Appropriate descriptive statistics were used as applicable. Continuous variables were described through mean ± standard deviation or median with interquartile range (IQR). A chi-square test was applied to find out the association of psychological distress with other variables. P < 0.05 was taken as significant.
RESULTS
Sociodemographic characteristics of the study participants
Among 340 study participants, the mean age was 22.78 years (±3.43 years). Males comprised 69.4% of the study participants. The majority were Hindus (76.2%), and 66.8% lived in urban areas. About 55.3% lived on hostel premises, and the majority (83.8%) were unmarried. The median per capita income of the participants was 15000 INR (IQR = 6616.50–30,000 INR). Approximately 86% of the study participants belonged to the nuclear family, and 233 (68.5%) study participants belonged to Class I socioeconomic status.9 Sociodemographic characteristics of the study participants are shown in Table 1.
| Variables | Categories | Frequency (%) |
|---|---|---|
| Age (in completed years) | 18–22 | 195 (57.4) |
| 23–27 | 117 (34.4) | |
| ≥28 | 28 (8.2) | |
| Gender | Male | 236 (69.4) |
| Female | 104 (30.6) | |
| Religion | Hinduism | 259 (76.2) |
| Islam | 74 (21.8) | |
| Christianity | 7 (2.0) | |
| Type of permanent residence | Urban | 227 (66.8) |
| Rural | 113 (33.2) | |
| Present residence | Hostel | 188 (55.3) |
| Day scholar | 152 (44.7) | |
| Marital status | Unmarried | 332 (97.6) |
| Married | 8 (2.4) | |
| Family type | Nuclear | 292 (85.9) |
| Joint | 48 (14.1) | |
| Socioeconomic status (as modified BG Prasad scale 2024) | Class I | 233 (68.5) |
| Class II | 43 (12.6) | |
| Class III | 17 (5.0) | |
| Class IV | 31 (9.1) | |
| Class V | 16 (4.7) |
Behavioral characteristics of the study participants
Substance usage was detected among 28 (8.2%) of the study participants, among which tobacco smoking was the most common substance identified (n = 25). Smokeless tobacco usage was detected among 11 study participants. Alcohol usage was detected among three study participants. Smartphone usage was detected among all the study participants. The median average screen time detected among the study participants was 5 h (IQR = 4–7 h).
Psychological distress among the study participants
The mean scores of the depression subscale in DASS-21 were 7.67 ± 5.72. Depression was present among 109 (32.0%) participants. Moderate levels of depression were present in 39 (11.5%) participants, while severe levels of depression were detected in 13 (3.8%) participants. The anxiety scores showed a median value of 6 (IQR = 4–9). Anxiety was present among 138 (40.5%) study participants. Severe anxiety was detected among 23 (6.8%) participants, while 6 (1.8%) were suffering from extremely severe levels of anxiety. The stress subscale showed a median value of 7 (IQR = 4–11). The presence of stress was detected among 46 (13.5%) participants. Moderate and severe levels of stress were detected among 9 (2.6%) and 5 (1.5%) participants, respectively [Figure 1].
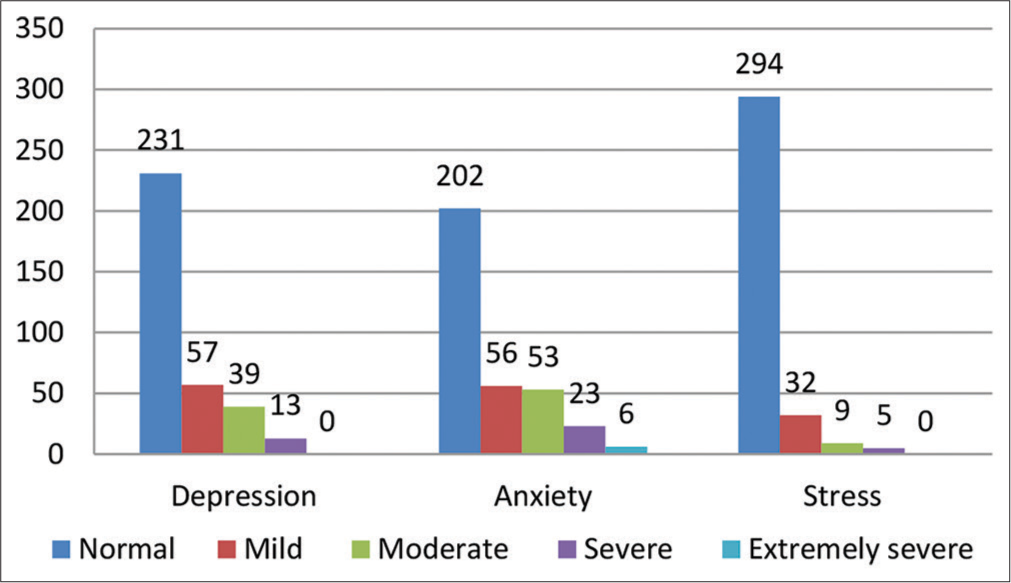
- Multiple bar diagram showing the distribution of different domains of psychological distress as assessed by depression, anxiety, and stress scale-21 among the study participants (n = 340).
Factors associated with the presence of psychological distress among the study participants
The presence of depression among the study participants was found to be significantly associated with age, as there was a significant difference in the presence of depression across the age groups (χ2 = 10.4, df = 1, P = 0.002). Females had higher chances of suffering (49% for females versus 36.9% for males), and this association was found to be statistically significant (χ2 = 4.437, df = 1, P = 0.035). In addition, participants of socioeconomic status below Class I had higher anxiety levels (χ2 = 4.154, df = 1, P = 0.042). Gender and substance usage had statistically significant association with the presence of stress among the study participants [Table 2].
| Variables | Categories | Depression present n (%) |
Inferential statistics |
Anxiety present n (%) |
Inferential statistics |
Stress present n (%) |
Inferential statistics |
|---|---|---|---|---|---|---|---|
| Age | ≤22 years (n=195) | 76 (39.0) |
χ2=10.4 df=1 P=0.002 |
86 (44.1) | χ2=2.342 df=1 P=0.126 |
30 (15.4) | χ2=1.345 df=1 P=0.246 |
| >22 years (n=145) | 33 (28.8) | 52 (35.9) | 16 (11.0) | ||||
| Gender | Males (n=236) | 78 (33.1) | χ2=0.349 df=1 P=0.555 |
87 (36.9) |
χ2=4.437 df=1 P=0.035 |
24 (10.2) |
χ2=7.445 df=1 P=0.006 |
| Females (n=104) | 31 (29.8) | 51 (49.0) | 22 (21.2) | ||||
| Religion | Hinduism (n=259) | 87 (33.6) | χ2=1.171 df=1 P=0.279 |
108 (41.7) | χ2=0.556 df=1 P=0.456 |
33 (12.7) | χ2=0.577 df=1 P=0.447 |
| Others (n=81) | 22 (27.2) | 30 (37.0) | 13 (16.0) | ||||
| Socioeconomic status | Class I (n=233) | 72 (30.9) | χ2=0.455 df=1 P=0.5 |
86 (36.9) |
χ2=4.154 df=1 P=0.042 |
26 (11.2) | χ2=3.557 df=1 P=0.059 |
| Below class I (n=107) |
37 (34.6) | 52 (48.6) | 20 (18.7) | ||||
| Residence | Rural (n=113) | 39 (34.5) | χ2=0.468 df=1 P=0.45 |
50 (44.2) | χ2=0.940 df=1 P=0.332 |
15 (13.3) | χ2=0.009 df=1 P=0.923 |
| Urban (n=227) | 70 (30.8) | 88 (38.8) | 31 (13.7) | ||||
| Substance usage | Absent (n=312) | 96 (30.8) | χ2=2.893 df=1 P=0.089 |
126 (40.2) | χ2=0.065 df=1 P=0.799 |
38 (12.2) |
χ2=5.901 df=1 P=0.015 |
| Present (n=28) | 13 (46.4) | 12 (42.9) | 8 (28.6) | ||||
| Average Screen time | ≤5 h (n=182) | 59 (32.4) | χ2=0.023 df=1 P=0.908 |
76 (41.8) | χ2=0.222 df=1 P=0.637 |
28 (15.4) | χ2=1.152 df=1 P=0.283 |
| >5 h (n=158) | 50 (31.6) | 62 (39.2) | 18 (11.4) |
Bold values indicate statistically significant association (P<0.05). df: Degrees of freedom
DISCUSSION
This study made a unique attempt in Kolkata by assessing the presence of anxiety, depression, and stress among medical students in a medical college in Kolkata and eliciting its associated factors. The validated DASS-21 was used to assess the three domains of psychological distress among medical students and interns. Depression, anxiety, and stress were present among 109 (32.0%), 138 (40.5%), and 46 (13.5%) participants, respectively. Similar findings were reported in a study conducted in a medical college in Northern India by Taneja et al., where the magnitude of depression, anxiety, and stress assessed similarly through DASS-21 was 32%, 40.1%, and 43.8%, respectively.10 Sarkar et al., in their systematic review of depression, anxiety, and stress among Indian medical students, estimated the pooled prevalence of depression, anxiety, and stress to be 39.2%, 34.5%, and 51.3%, respectively.7 Raja et al. utilized the DASS-21 among medical students in a medical institute in southern India and found the prevalence of depression, anxiety, and stress to be 59%, 43%, and 11%, respectively.5 Another systematic review and meta-analysis among undergraduate medical students in India by Dutta et al. estimated the pooled prevalence of depression to be 50%.11
In the present study, females were detected as having higher levels of stress and anxiety compared to females, and this association was found to be statistically significant. Ahad et al. conducted a study among undergraduate dental students in India and detected female gender as an independent indicator of stress.12 Rajanayagam et al. conducted a study among 1st-year undergraduate medical students in the southern state of Tamil Nadu, India, and detected females having higher chances of stress as compared to males.13 In the present study, substance usage was detected as an important predictor of stress among the study participants. This might have been implicated that substance usage is sometimes used as a means to cope with stressful conditions. This often initiates a vicious cycle of substance usage and stressful circumstances, which lead to the progression of addiction among the vulnerable population. The above finding thus necessitates the importance of taking care of the mental health and well-being of medical students.
Limitations
Certain limitations to our study exist. Since this study was cross-sectional, the causal relationship between the variables could not be established. Some of the answers derived were recall-based, so bias might be possible. Moreover, as this study was single institution-based, the actual scenario of mental health and distress of medical students might vary from the actual scenario. Large multicentric studies are thus needed in this domain.
CONCLUSION
The present study detected significant levels of psychological distress among the study students. Medical students are the future backbone of the medical fraternity and health-care system of India. Hence, utmost care should be taken to better their mental health and well-being. Awareness generation and one-to-one counseling sessions through motivation should be conducted, especially for the vulnerable participants. Parents and peers can act as buffers to help those students cope with stressful circumstances.
Ethical approval
The research/study was approved by the Institutional Review Board at the Institutional Ethics Committee for Human Research, Medical College, Kolkata, number 2237, dated January 2024.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Mental Health Status of the General Population, Healthcare Professionals, and University Students During 2019 Coronavirus Disease Outbreak in Jordan: A Cross-sectional Study. Brain Behav. 2020;10:e01730.
- [CrossRef] [PubMed] [Google Scholar]
- Medical Student Psychological Distress and Mental Illness Relative to the General Population: A Canadian Cross-sectional Survey. Acad Med. 2019;94:1781-91.
- [CrossRef] [PubMed] [Google Scholar]
- Impact of Action Video Gaming Behavior on Attention, Anxiety, and Sleep among University Students. Psychol Res Behav Manag. 2022;15:151-60.
- [CrossRef] [PubMed] [Google Scholar]
- Suicide Deaths among Medical Students, Residents and Physicians in India Spanning a Decade (2010-2019): An Exploratory Study Using on Line News Portals and Google Database. Int J Soc Psychiatry. 2022;68:718-28.
- [CrossRef] [PubMed] [Google Scholar]
- Prevalence of Depression, Anxiety and Stress among Private Medical College Students in South India: A Cross-sectional Study. J Edu Health Promot. 2022;11:373.
- [CrossRef] [PubMed] [Google Scholar]
- Psychology Foundation of Australia. 2018. Available from: http://www2.psy.unsw.edu.au/dass [Last accessed on 2024 Jan 20]
- [Google Scholar]
- A Systematic Review of Depression, Anxiety, and Stress among Medical Students in India. J Mental Health Hum Behav. 2017;22:88-96.
- [Google Scholar]
- Manual for the Depression Anxiety and Stress Scales. (2nd ed). Sydney: Psychology Foundation; 1995.
- [CrossRef] [Google Scholar]
- Updated B. G. Prasad Scale for Socioeconomic Status Classification for the Year 2024. Indian J Pediatr. 2024;91:643.
- [CrossRef] [PubMed] [Google Scholar]
- Assessment of Depression, Anxiety, and Stress among Medical Students Enrolled in a Medical College of New Delhi, India. Indian J Soc Psychiatry. 2018;34:157-62.
- [CrossRef] [Google Scholar]
- Prevalence of Depression Among Undergraduate Medical Students in India: A Systemic Review and Meta-Analysis. Cureus. 2023;15:e33590.
- [CrossRef] [Google Scholar]
- Factors Affecting the Prevalence of Stress, Anxiety, and Depression in Undergraduate Indian Dental Students. J Educ Health Promot. 2021;10:266.
- [CrossRef] [PubMed] [Google Scholar]
- Prevalence of Anxiety Depression and Stress among First Year Medical Students in Tamil Nadu. Bioinformation. 2023;19:649-54.
- [CrossRef] [PubMed] [Google Scholar]






